This week, March 6 – 13, is National Sleep Awareness Week, so it’s a good time to review healthy sleep habits. I see a lot of adults and teens in my clinic who are chronically tired and have troubles sleeping — both falling asleep and staying asleep.… Read the rest
Category Archives: Wellness
Don’t Skip Breakfast! Here’s Why.
Did you know that the U.S. Center for Disease Control predicts that one third of all Americans will have diabetes by the year 2050? This scary statistic is not just an American phenomenon; many Western countries’ modernized diets have led to a diabetes epidemic.… Read the rest
Rubber Ducky You’re The One — To Cause Diabetes and Cancer?
My boys are now both over two years old, but they still like the occasional chew on their toys, which are mostly made of plastic. Rubber duckies, Lego men, Brio trains — it’s still a ton of fun to put in their mouths if it makes mommy and daddy really mad.… Read the rest
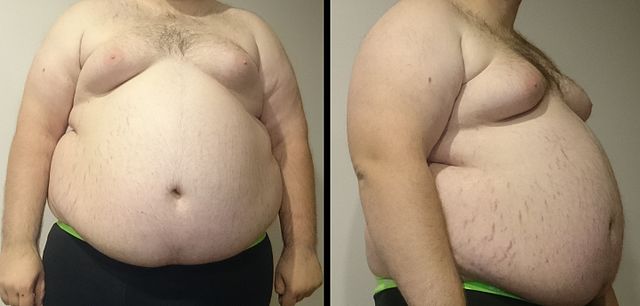
Obesity in Childhood: How Can We Stop the Pandemic?
Curing a Cough: What’s the Best Medicine?
Coughing from a cold or flu is probably the most frustrating symptom we can have — for children, their parents, and even the doctor treating them. Why? Because there’s honestly very little that we can do to treat it. That’s a hard pill to swallow, and it’s especially humbling for me as a family physician.… Read the rest
Why I Became A Family Doctor
I am a family medicine doctor – but that is only a small part of who I am. Father, husband, photographer, social media guru, writer, singer — these are only a few of the many ways I define myself. But when I am on my deathbed, hopefully many decades from now, and looking back on my life, what will I list as my top accomplishments?… Read the rest






